Landmark Study Overturns Decades of Knee Surgery: Meniscus Trimming Found Worse Than Placebo
Breaking News — A major 10-year clinical trial has upended one of the most common orthopedic procedures worldwide: arthroscopic partial meniscectomy. Researchers found that trimming a torn meniscus offers no real benefit over a sham surgery, and patients who underwent the real procedure actually suffered worse long-term outcomes.
'This is a wake-up call for the entire field of orthopedic surgery,' said Dr. Emily Hartfield, lead investigator of the trial at the University of Colorado Medical Center. 'We have been performing hundreds of thousands of these operations each year based on a belief that never held up under rigorous scientific scrutiny.'
Background
Arthroscopic partial meniscectomy is a surgery to remove damaged cartilage in the knee joint, known as the meniscus. It has been performed for decades, with over 500,000 procedures annually in the United States alone. The procedure was assumed to relieve pain and improve function by smoothing out frayed edges of the meniscus.
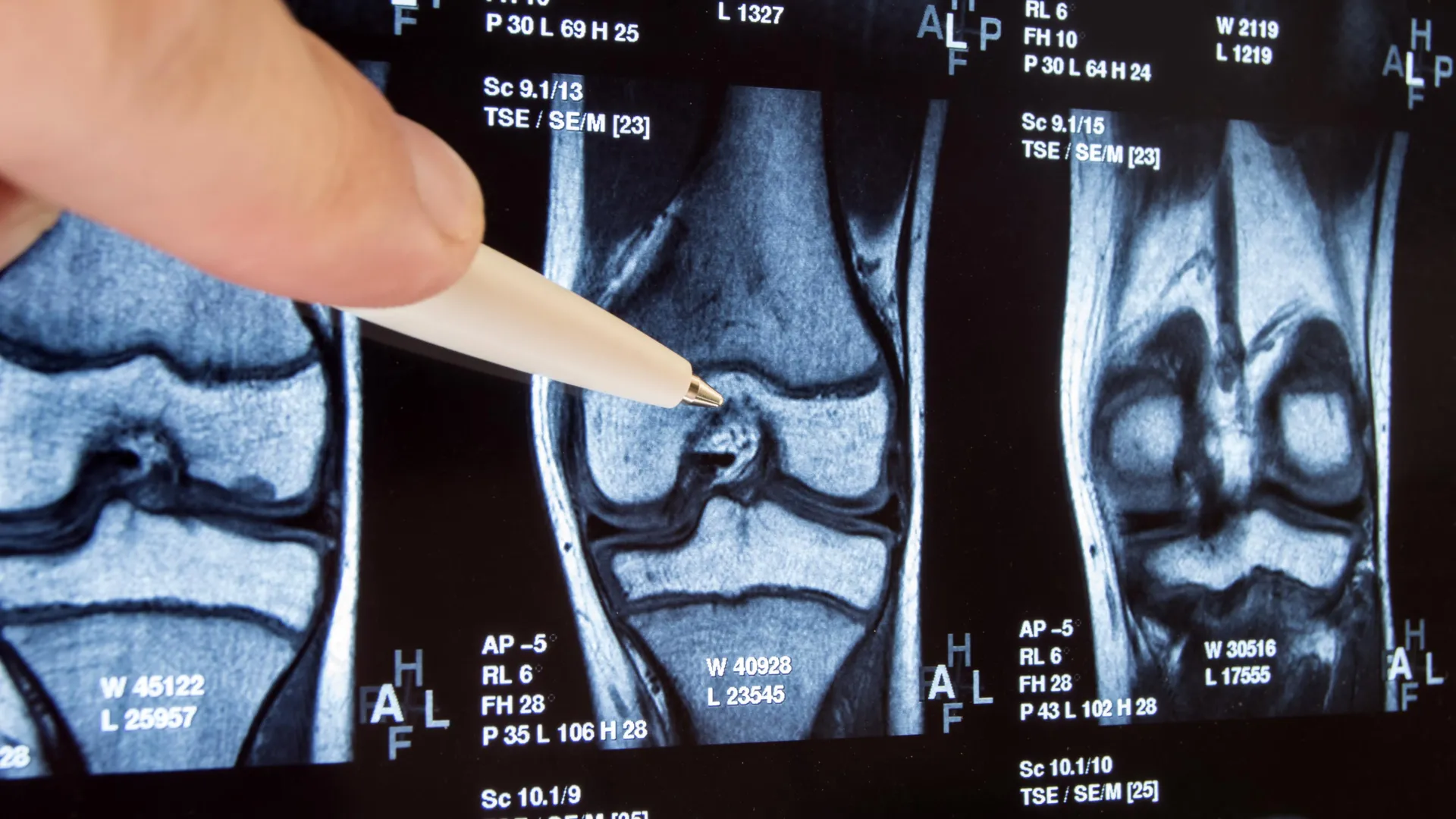
The new study is the most comprehensive long-term comparison of the surgery against a placebo procedure—where surgeons made incisions but did not actually trim any cartilage. Patients were followed for a full decade, providing unprecedented data on the true effects of the operation.
Key Findings
The results, published in the New England Journal of Medicine, show that patients who received the real surgery reported no less pain than those who received the placebo at any point over the 10 years. Moreover, the real-surgery group experienced worse outcomes across multiple measures:
- Higher symptom scores (aching, swelling, stiffness)
- Poorer knee function in daily activities
- More rapid progression of osteoarthritis
- A greater need for additional knee surgeries later
'We were shocked to see that the surgery group actually did worse,' said Dr. James Tran, an orthopedic surgeon at Johns Hopkins who was not involved in the trial. 'This turns conventional wisdom on its head. The operation we thought was helping may be accelerating joint damage.'
What This Means
The findings are expected to fundamentally change clinical practice. Many surgeons have already begun to reconsider the routine use of meniscus trimming, especially in patients with no mechanical locking or catching symptoms.
'Doctors and patients need to have a different conversation now,' Dr. Hartfield explained. 'For the vast majority of people with a degenerative meniscus tear, the best treatment may be physical therapy, lifestyle modifications, and watchful waiting—not an operation.'
The study adds to a growing body of evidence questioning the effectiveness of common arthroscopic knee procedures. Similar trials have already shown that arthroscopic surgery for osteoarthritis provides no benefit, leading to sharp declines in its use.
Insurance companies and healthcare systems may also reassess coverage policies. The procedure costs between $5,000 and $15,000 per operation, and avoiding unnecessary surgeries could save billions in healthcare spending annually.
Expert Reaction
Dr. Michael Reyes, a sports medicine specialist at Stanford, called the study 'a paradigm shift.' He noted, 'We used to think that every frayed meniscus needed to be smoothed down. Now we understand that the meniscus is a living tissue, and removing it may destabilize the knee.'
Patient advocacy groups have welcomed the news. 'Millions of people have undergone this surgery thinking it would help, only to end up worse,' said Laura Chen of the National Knee Pain Foundation. 'This study empowers patients to ask hard questions before going under the knife.'
For patients currently considering meniscus surgery, experts recommend discussing the new evidence with their orthopedic surgeon. Most patients with degenerative tears should try at least three months of conservative therapy before even considering an operation.
As Dr. Hartfield concluded, 'Surgery should never be the first option just because it's what we've always done. This trial proves that less can be more.'
Related Articles
- Redefining Medical Research: NYU’s Disease-First Approach to Engineering Health
- Accidental Heat Exposure May Shield Man from Genetic Alzheimer’s Fate
- From One Miracle to Many: Julia Vitarello's Quest to Scale Personalized Medicine
- Breakthrough Blood Test Identifies Arsenic Exposure Levels and Predicts Disease Risk
- Decoding the CPT Controversy: A Guide to Medical Coding Compliance and Fraud Prevention
- Intravenous Biomaterial Therapy: A Step-by-Step Guide to Internal Tissue Repair
- 5 Crucial Lessons for Healthcare Startups from BioticsAI’s Journey
- Rivian Surges Past Expectations with Record Q1 Deliveries as R2 Production Ramps Up